 I was first alerted to the differences in how people with autism learn through my contact with George, a 13-year-old boy. Prior to this, I had never really had direct contact with anyone with autism. I had seen George a few times for OHE sessions, and his younger sister and mother had also attended and been actively involved in the sessions.
I was first alerted to the differences in how people with autism learn through my contact with George, a 13-year-old boy. Prior to this, I had never really had direct contact with anyone with autism. I had seen George a few times for OHE sessions, and his younger sister and mother had also attended and been actively involved in the sessions.At the first review appointment with George it seemed that there had been no improvement. I requested that he returned for a further review, and he naturally felt quite negative about this. It was at the start of the second review appointment that George’s mum asked for a quiet word away from her children. She wanted to ask how we could make her son feel more positive and motivated, as he was getting frustrated at home. It was at this point that she mentioned that George was autistic. We had no record of this in his medical history or notes, because his mom had never thought it a relevant thing to tell us.
Any of you who have had experience of dealing with autism will know that it is indeed very relevant, especially when giving oral health education advice.
According to the National Autism Society:
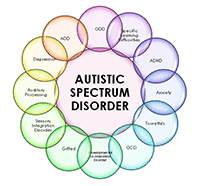
"Autism is a lifelong developmental disability that affects how a person communicates with, and relates to, other people. It also affects how they make sense of the world around them."
I explained to George’s mum that the way I communicated with George needed to be adjusted. She asked whether I could set him goals, as she had found this to be a successful strategy for achieving various tasks at home - so that's exactly what I did. The first goal I set for George was just to brush for longer. We discussed a few different things that could help him with this. These were:
1. A traditional sand timer that runs for two minutes.
2. A tooth-brushing app on a smartphone or tablet.
3. Listening to his favourite song while brushing (the average song length is three minutes).
There is actually an app called ‘Brush DJ’ which links you to iTunes and plays your favourite music while timing brushing. Alternatively, for younger children, the Aquafresh app is very good. The child gets to choose a ‘Nurdle’ for their profile. As they brush, they earn rewards - the rewards allow them to alter their Nurdle, such as by dressing it up!
The next time I saw George, there was an improvement. He had been using disclosing tablets at home, but didn't like the Brush DJ app. Instead, he had decided to use a stopwatch in the bathroom for three minutes, twice a day. We also discussed a new goal - actually looking at what he was doing with the toothbrush, including the position of the brush. He was currently using a manual toothbrush as he didn't like the sensation of an electric toothbrush, but he was using large sweeping movements. So we worked on making those movements smaller. He now had two goals:
1. To brush for three minutes, twice a day.
2. To use smaller side-to-side movements with his toothbrush.
Six weeks later, there had been further improvement. The situation was by no means perfect, and we still had more work to do; but each time I saw George I made sure praise and encouragement were given, and reinforced the goals we had set. His general oral health had obviously improved, as there was no longer bleeding when he brushed, and the gingiva appeared generally healthier. We had made huge progress from where we originally started, but this had only been made possible through gaining an understanding of George’s autism and the way I needed to tailor his learning experience – and, indeed, alter my language and approach to his care.
Here is some advice from the National Autism Society [1]:
Your language
Use clear, simple language with short sentences.
People with an ASD (Autistic Spectrum Disorder) tend to take everything literally. Thus, if you say "It will only hurt for a minute," they will expect the pain to have gone within a minute.
Make your language concrete and avoid using idioms, irony, metaphors and words with double meanings, eg "It's raining cats and dogs out there." This could cause the patient to look outside for cats and dogs.
Give direct requests, eg "Please stand up." If you say, "Can you stand up?" this may result in the person staying seated, or the answer "Yes", as the patient may not understand you are asking them to do something.
Check that the patient has understood what you have said - some people with an ASD may speak clearly, but can lack full understanding.
Avoid using body language, gestures or facial expressions without verbal instructions. These may not be understood.
Ask for the information you need. A person with an ASD may not volunteer vital information without being asked directly.
Don't be surprised if the patient doesn't make eye contact, especially if he or she is distressed. Lack of eye contact does not necessarily mean they are not listening to what you are saying.
Allow the patient extra time to process what you have said.
Don't assume that a non-verbal patient cannot understand what you are saying.
People with an ASD may find it difficult to understand another person's perspective. They may not understand what you intend to do, but may expect you to know what they are thinking.
People with an ASD may not understand personal space. They may invade your personal space or need more personal space than the average person.
Since helping George, I have found myself working closely with other children who suffer from autism, Asperger syndrome, dyspraxia and other specialist educational needs. I'm happy to say that I have witnessed some real, positive improvements. I have also received a huge amount of thanks from very grateful parents, who had been struggling to motivate their children prior to attending OHE sessions.
In summary, when dealing with special educational needs, remember the following;
• Use simple, clear language.
• Ask direct questions.
• Only give one or two simple pieces of information - don't overload the person or over-complicate things.
I think that it is really important for oral health educators to ensure that some of their CPD reading is dedicated to learning all about special educational needs, and to ensure that we are not only delivering the right oral health messages, but are doing so in the correct manner so that everyone benefits from preventative advice.
References
[1] http://www.autism.org.uk/working-with/health/patients-with-autism-spectrum-disorders-guidance-for-health-professionals.aspx